

Kate is in the midst of packing up her blue and green house in Saint John, NB for a new adventure in Antigonish, NS (population 4,200, whoo!). She has two wonderful small people in her life, and loves reading, biking, swimming and dancing (badly!).
Simple wellness in a frantic world.
Home » Blog » Health & Wellness » Pregnancy, Birth, & Breastfeeding » Baby-Catcher: A Memoir-ish Account of a Midwifery Journey {Part Three}
Updated: | 3 Comments | This post may contain affiliate links. Click here for our full disclosure.



Kate is in the midst of packing up her blue and green house in Saint John, NB for a new adventure in Antigonish, NS (population 4,200, whoo!). She has two wonderful small people in her life, and loves reading, biking, swimming and dancing (badly!).
Share the love!
Beth is the creator here at Red & Honey. Mom of four, wife of one, and proud redhead. Sushi and tex-mex lover, fan of adventure, books, natural health talk, and pyjamas. INFP and Type 4 enneagram. Allergic to small talk. And, if you haven't figured it out already, #nerd. Read more posts by Beth.
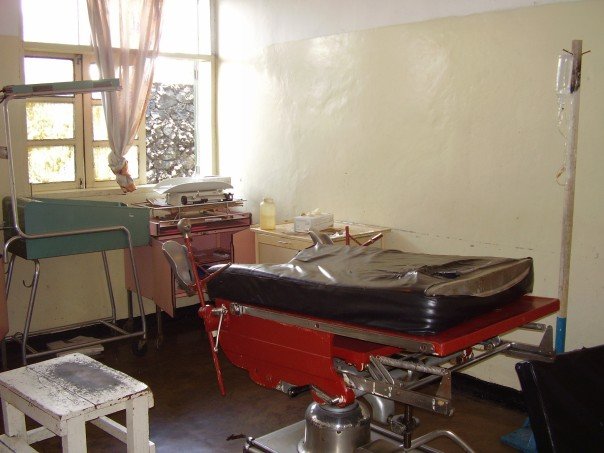
 Hospital Birth vs. Home Birth: My Small-Town Dilemma
Hospital Birth vs. Home Birth: My Small-Town Dilemma Uninhibited Breastfeeding in Public {Is It Obscene and Inappropriate?}
Uninhibited Breastfeeding in Public {Is It Obscene and Inappropriate?} Breastfeeding Battles: Naomi’s Story {Part Two}
Breastfeeding Battles: Naomi’s Story {Part Two} Why Having a Doula Was One of the Best Decisions I’ve Ever Made
Why Having a Doula Was One of the Best Decisions I’ve Ever Made Everett’s 47-hour Labour & Birth Story (Part Two)
Everett’s 47-hour Labour & Birth Story (Part Two) Baby-Catcher: A Memoir-ish Account of a Midwifery Journey {Part Two}
Baby-Catcher: A Memoir-ish Account of a Midwifery Journey {Part Two} 7 Ways to Prepare for a Successful VBAC
7 Ways to Prepare for a Successful VBAC Why I’m a Passionate Co-Sleeping Advocate
Why I’m a Passionate Co-Sleeping AdvocateThis site uses Akismet to reduce spam. Learn how your comment data is processed.
About Me
I’m a mom of four with an obsession for all things natural health, but I’m driven by wellness, not perfection. I’m an eternal optimist, a non-conformist, and a classic INFP. When I was 19, I married my total-opposite hubby, who is an ESTJ. This remains both the craziest and the best decision we’ve ever lived to tell about. I can always be bribed with sushi or tex-mex, and I love to embarrass my husband by cranking the music and dancing (badly) in the passenger seat.
Pour a cup and shop my favorite healthy living resources.
Browse My Shop
Are you hungry for a breakfast revolution in your house that won't leave you hungry an hour later? Need some new breakfast recipes under your belt that are made with real-food, nutrient-dense (and gluten-free) ingredients? The Breakfast Revolution e-cookbook is your solution.

This refreshingly honest and helpful eBook will encourage and equip you to take back your family dinner hour, and transform it into an enjoyable experience once again. And you can do it within the framework of a nourishing, real-food diet. (Yes, really!)

COOK. EAT. REPEAT. But first, figure out what to put in your cart. The grocery store can be a confusing place – what’s legitimately healthy, and what’s simply masquerading as healthy in an attempt to manipulate you? Get my best advice and tricks from a decade of experience, all in this book.



becoming a doula in ontario
This theme is simply matchless :), it is pleasant to me))) la dona mobile
cate
I just happened upon your blog! What an amazing experience! I agree with the comment above this definitely seems like a perfect fit for you! What a wonderful experience you will have!
mommyrose
That’s awesome Kate. 🙂 Will be praying for you through your midwife journey. Definitely sounds like it is God’s calling on your life!
Krista